Have you ever felt so heavy-hearted that you couldn't tell if it was just the pain of losing someone or something deeper taking hold? You are not alone in this confusion. Grief is the natural emotional response to loss, characterized by waves of sadness interspersed with positive memories, while Depression, clinically known as Major Depressive Disorder, is a persistent mental health condition marked by continuous low mood and loss of interest. The lines between them often blur, but understanding the distinction is crucial for finding the right path to healing. Getting this wrong can mean missing out on effective treatment or, worse, being treated for a condition you don’t have.
Understanding the Core Differences
To navigate these waters, we first need to look at what drives each experience. Grief is tied directly to a specific event-usually the death of a loved one. It is an attachment-based reaction. When you grieve, your thoughts circle back to the person you lost. You might feel intense longing, anger about the unfairness of their passing, or deep sorrow. But here is the key: those painful feelings usually come in waves. One moment you might be crying, and ten minutes later, you might smile at a funny memory of them. This fluctuation is normal.
Depression, on the other hand, is more like a flatline. It is not necessarily triggered by a single event, though life stressors can contribute. The defining feature of Major Depressive Disorder is a persistent state of low mood and anhedonia (loss of pleasure) lasting at least two weeks. Unlike grief, where memories of the deceased can bring comfort, depression often strips away the ability to feel good about anything. People with depression frequently report feeling worthless or guilty without a clear reason. They don’t just miss someone; they feel empty inside, regardless of who is around them.
The Diagnostic Criteria: What Experts Look For
Clinicians rely on specific guidelines to distinguish between these states. The DSM-5 is the Diagnostic and Statistical Manual of Mental Disorders, the standard classification of mental disorders used by mental health professionals in the United States plays a huge role here. In its updates, particularly with the inclusion of Prolonged Grief Disorder as a distinct diagnosis requiring intense yearning and preoccupation with the deceased for at least six months, the medical community has made it clearer that grief isn't just "sadness."
If you are looking at the checklist for Major Depressive Disorder, doctors look for five or more symptoms over two weeks. These include significant weight changes, insomnia or sleeping too much, fatigue, difficulty concentrating, and recurrent thoughts of death. Notice that "feeling sad" is just one part of it. In contrast, Prolonged Grief Disorder focuses heavily on the relationship to the loss. According to the World Health Organization's ICD-11, this involves persistent yearning, emotional numbness, and bitterness specifically related to the death. If your pain is centered entirely on the absence of the person, it leans toward grief. If your pain is a generalized sense of worthlessness and hopelessness about life itself, it leans toward depression.
| Feature | Grief / Prolonged Grief | Major Depression |
|---|---|---|
| Focus of Thoughts | Centered on the deceased person | Generalized negative self-view |
| Mood Pattern | Waves of pain mixed with positive memories | Persistent low mood without respite |
| Self-Worth | Generally preserved; guilt may relate to the loss | Feelings of worthlessness or excessive guilt |
| Social Response | Often seeks connection and support | Tends to withdraw and isolate |
| Duration Criteria | Intense symptoms >6 months post-loss | Symptoms present >2 consecutive weeks |
How Social Support Plays a Role
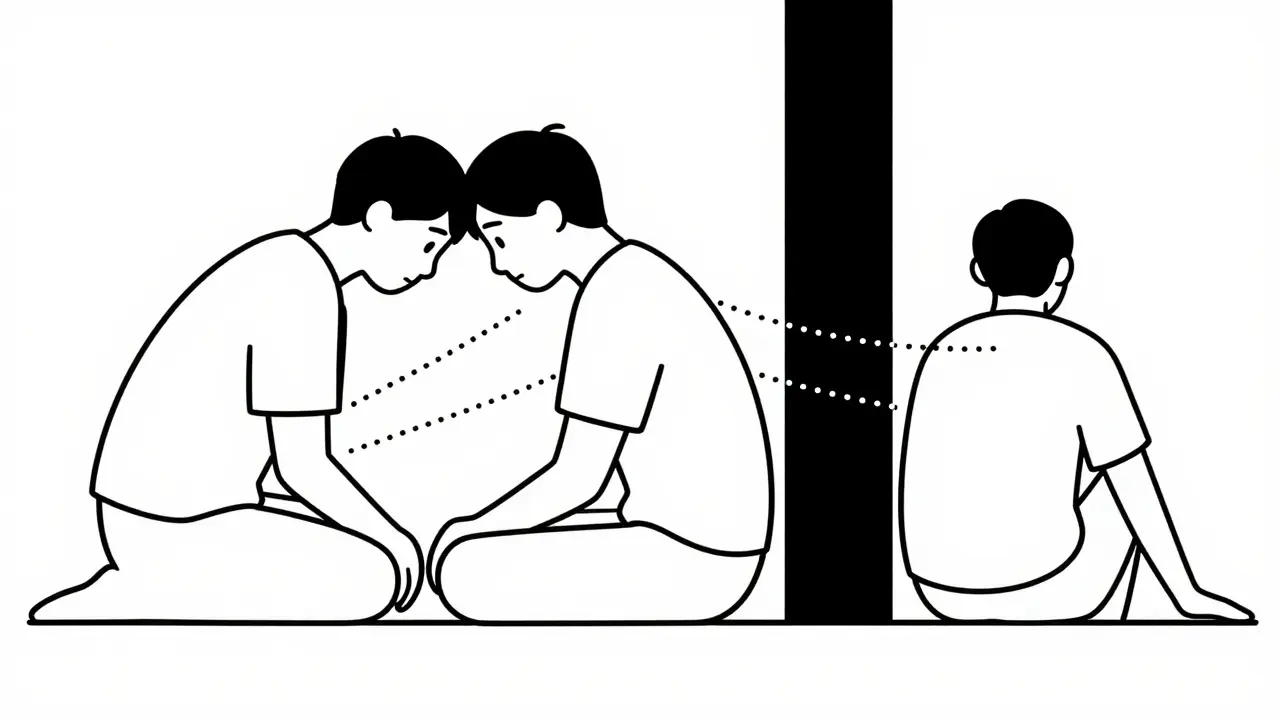
One of the most telling signs in real life is how you interact with others. Dr. Michael Miller from Harvard Medical School points out that people experiencing grief typically respond well to social support. You might find yourself wanting to talk about the person you lost, sharing stories, or just sitting with friends who understand. There is a communal aspect to grief. It connects us to our history and our relationships.
Depression works differently. It acts like a wall. A study published in *Depression and Anxiety* found that while most bereaved individuals actively seek support, many with depression avoid it. They might feel like a burden or simply lack the energy to engage. If you notice that someone is pushing everyone away, refusing to leave their room, or unable to connect even when loved ones try hard, that isolation is a red flag for depression rather than typical grief.
Treatment Paths: Why Diagnosis Matters
You cannot treat grief and depression with the same toolbox. Using the wrong approach can stall recovery. For uncomplicated grief, time and support are often the best medicine. The National Institute for Health and Care Excellence (NICE) guidelines suggest that antidepressants are generally not recommended for pure grief because the brain’s chemistry isn’t the primary issue-it’s the processing of loss. Most people see significant improvement within six months through natural coping mechanisms and therapy focused on acceptance.
However, if Complicated Grief Treatment is a specialized psychotherapy developed by Columbia University researchers to help patients process loss and rebuild life is needed, it focuses on dual-process therapy-helping you oscillate between confronting the loss and avoiding it until you can integrate it into your life. On the flip side, depression often requires a different intervention. Cognitive Behavioral Therapy (CBT) combined with medications like SSRIs (e.g., sertraline) is the gold standard. Research shows that while grief responds best to targeted talk therapy, depression benefits significantly from medication to correct neurotransmitter imbalances. Mixing these up can lead to frustration-for instance, prescribing antidepressants to someone whose main struggle is unresolved grief might mask symptoms without addressing the core wound.
Supporting Someone Else: Practical Steps
If you are trying to help a friend or family member, your role is vital but tricky. First, listen without judgment. Don’t rush to fix their pain. Ask open-ended questions like, "How are you feeling today?" rather than assuming you know. Pay attention to their language. Are they talking about the person they lost? Or are they talking about how useless they feel? The former suggests grief; the latter suggests depression.
Encourage small steps. For grief, this might mean visiting a memorial site or looking at photos together. For depression, it might mean helping them shower, eat a balanced meal, or schedule a doctor’s appointment. Monitor for danger signs. If you hear statements about wanting to die or feeling like a burden, take them seriously. This is especially critical in depression, where suicide risk is higher. In both cases, professional help is key. Encourage them to see a therapist who specializes in either bereavement or mood disorders. The Association for Death Education and Counseling lists certified counselors who can guide you through this complex terrain.
When to Seek Professional Help
There is no strict timeline for grief, but there are warning signs. If intense symptoms persist beyond six months and significantly impair daily functioning-such as inability to work, maintain hygiene, or care for dependents-it may be Prolonged Grief Disorder. If low mood, lack of interest, or physical symptoms last for more than two weeks and affect all areas of life, it could be Major Depressive Disorder. Remember, it is possible to have both. Studies show that a small percentage of people experience comorbid conditions. In such cases, a multidisciplinary approach involving both psychiatric medication and grief-specific therapy is often necessary.
Don't wait for things to get worse. Early intervention improves outcomes. Whether it's a counselor, a psychiatrist, or a support group, reaching out is a sign of strength, not weakness. Your mental health is too important to guesswork. Get the right diagnosis, follow the right treatment plan, and allow yourself the space to heal.
Can grief turn into depression?
Yes, it is possible for grief to co-occur with or trigger depression. While grief itself is a natural response to loss, the stress and trauma involved can sometimes lead to Major Depressive Disorder, especially if the individual has a history of depression or lacks strong social support. However, they remain distinct conditions with different underlying causes and treatments.
How long does normal grief last?
There is no set timeline for grief, as it varies greatly from person to person. However, clinical guidelines often use six months as a benchmark. If intense symptoms like overwhelming yearning, emotional numbness, or inability to function persist beyond six months after the loss, it may be classified as Prolonged Grief Disorder, which requires professional intervention.
What is the best treatment for prolonged grief?
The most effective treatment for Prolonged Grief Disorder is specialized psychotherapy, such as Complicated Grief Treatment (CGT). This therapy helps individuals process the loss, manage avoidance behaviors, and rebuild a meaningful life. Antidepressants are generally less effective for pure grief compared to their efficacy in treating major depression.
Is it normal to feel happy while grieving?
Absolutely. Experiencing moments of happiness, humor, or peace while remembering the deceased is a hallmark of normal grief. These positive emotions are interspersed with waves of sadness. In contrast, depression typically involves a persistent inability to feel pleasure or joy, regardless of external circumstances or memories.
Can I have both grief and depression at the same time?
Yes, comorbidity is possible. Some individuals experience the specific pain of loss alongside the generalized symptoms of major depression. In these cases, a healthcare provider may recommend a combination of therapies, including grief-focused counseling and possibly medication, to address both aspects of the condition effectively.
