Imagine waking up to find your child standing on a balcony or your partner trying to cook a meal in the middle of the night, completely unaware of where they are. For people living with parasomnia safety is not just a precaution-it's a necessity. These sleep disorders, which involve abnormal behaviors like sleepwalking or REM sleep behavior disorder, can turn a peaceful bedroom into a hazard zone in seconds. With injury rates hitting up to 38% among frequent sleepwalkers, the goal isn't to "cure" the episodes overnight, but to build a fail-safe environment where an episode can happen without resulting in a trip to the emergency room.
| Modification Area | Recommended Action | Primary Benefit |
|---|---|---|
| Bed Height | Lower bed to floor level | Eliminates fall-related injuries |
| Room Perimeter | 6-foot clear radius around bed | Prevents tripping and collisions |
| Windows/Doors | Secondary locks & electronic alarms | Prevents wandering outside the room |
| Flooring | High-density foam padding | Reduces impact injuries from falls |
Securing the Immediate Sleep Area
The area directly surrounding the bed is where most immediate injuries occur. Standard beds are usually 18 to 24 inches high, which is plenty of height to cause a sprain or a head injury during a confused arousal. One of the most effective moves is to lower the bed to floor level. By removing the frame and placing the mattress directly on the floor, you essentially eliminate the risk of a dangerous fall.
If a floor mattress isn't an option, installing padded bed rails is the next best step. Look for rails that extend at least 16 inches above the mattress. This prevents the "roll-out" effect where someone slides off the bed while in a semi-conscious state. However, the real danger often lies in what's around the bed. Create a 6-foot "no-fly zone" by removing all furniture, nightstands, and especially electrical cords or area rugs. These small items are the primary culprits for trips and falls during sleepwalking episodes.
For those who struggle with severe episodes, the Cleveland Clinic suggests adding 2-inch thick high-density foam padding along the walls within a 3-foot perimeter. It sounds extreme, but it turns a potential collision with a wall into a soft bounce, significantly reducing the risk of bruising or concussions.
Blocking Exits and Preventing Wandering
Once a person leaves the bed, the risk shifts from falling to wandering. This is particularly dangerous in multi-story homes. If you have the option, move the bedroom to the ground floor. Data shows that a staggering 92% of serious parasomnia injuries happen in upper-level bedrooms, usually involving stairs or balconies.
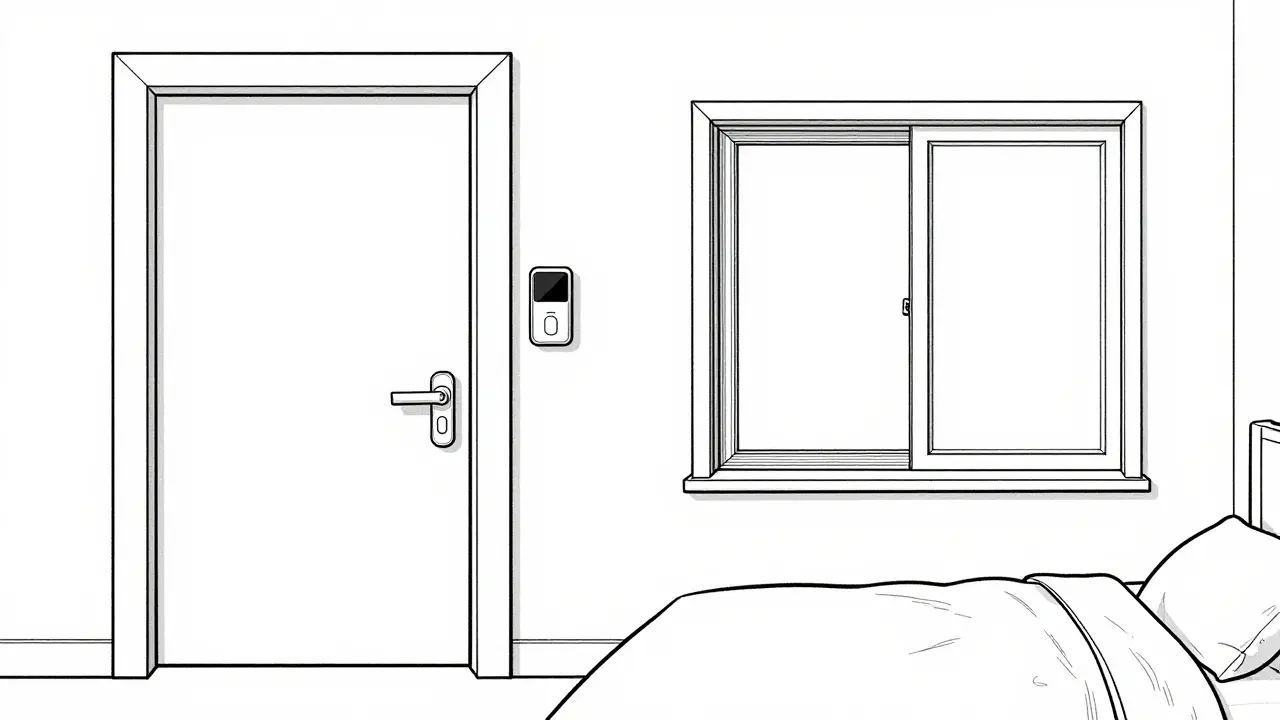
Windows need a double layer of security. Standard locks aren't always enough for someone in a state of confusional arousal. Install secondary locks on second-story windows that require about 10 pounds of force to operate. This keeps the window shut against unconscious attempts to open it, while still allowing someone to get out in case of a fire.
Door security is where technology becomes a lifesaver. Electronic door alarms-like the Sleep Guardian Pro-can alert caregivers the moment a door opens. The key is sensitivity; you want a device that triggers instantly so you can intervene before the person leaves the room. If you're shopping for these, avoid the ultra-cheap models. Medical-grade systems have far fewer false alarms, meaning you won't stop ignoring the buzzer after three nights of it going off for no reason.
Bedding Hacks and Physical Restraints
While you should never tie someone to a bed, you can use bedding to create a gentle "boundary." Some families have found success using full-length sleeping bags with armholes. This isn't about trapping the person, but rather creating a sensory barrier that can reduce the distance a person wanders and make them more likely to stay in the sleep zone.
If you're dealing with a child, involve them in the process. Let them pick the color of the floor padding or the sound of the alarm. When kids feel like they're helping build their "safety fort," they're much less anxious about the changes and more likely to follow the new routines.
Managing the Episode: What to Do and Avoid
When you catch someone in the middle of a parasomnia episode, your instinct is to shake them awake. Stop right there. Abruptly waking someone during a night terror or sleepwalking episode can trigger a violent reaction. They are essentially trapped between sleep and wakefulness; forcing them into the latter too quickly can cause a "fight or flight" response.
Instead, use a low, calm voice-keep it around 45-55 decibels. Gently guide them back to bed using short, simple directions. "You're okay, let's go back to bed" works far better than "Wake up! What are you doing?" Most episodes will terminate safely with this kind of gentle redirection.
For those whose episodes happen at the same time every night, try "scheduled awakenings." Keep a sleep diary for two weeks to find the pattern. Then, wake the person up gently 15 to 30 minutes before the typical episode start time. This disrupts the sleep cycle just enough to prevent the abnormal behavior from triggering.
Sleep Hygiene as a Preventive Shield
Physical barriers are your last line of defense; sleep hygiene is your first. Parasomnias are often triggered by fragmented sleep. To stabilize sleep architecture, stick to a strict schedule with no more than 30 minutes of variation in your wake-up and bedtime.
The environment plays a massive role. Keep your bedroom cool-between 60 and 67°F (15.6-19.4°C)-and maintain humidity between 40% and 60%. A room that is too hot or too stuffy can trigger the restlessness that leads to an episode.
Watch your intake. Caffeine should be avoided for 8 hours before bed, and alcohol-which might seem to help you fall asleep-actually fragments sleep and can make parasomnia episodes more severe. Finally, ditch the screens. Keeping electronics at least 10 feet away from the bed and avoiding them for two hours before sleep helps your brain transition more smoothly into deep sleep, reducing the chance of partial arousals.
Is it dangerous to wake a sleepwalker?
Yes, it can be. Abruptly waking someone can cause confusion, fear, and even violent reactions. It is much safer to use a calm, quiet voice to gently lead them back to their bed without fully waking them up.
Which floor is safest for someone with parasomnia?
The ground floor is the safest. Because a vast majority of serious injuries occur in upper-level bedrooms (due to stairs and windows), sleeping on the first floor removes the most critical risks.
Do bed alarms actually work?
Yes, they are highly effective for alerting caregivers. However, there is a big difference between consumer-grade and medical-grade alarms. Medical-grade systems have significantly lower false-alarm rates, making them more reliable for long-term use.
Can supplements help reduce episodes?
Some research suggests melatonin (2-5 mg) taken two hours before bed can reduce pediatric parasomnia frequency. However, you should always consult a doctor before starting supplements, especially for children.
How long does it take to set up these safety modifications?
Most people find that a full adaptation period takes about 2 to 4 weeks. This includes purchasing equipment, rearranging furniture, and getting the person accustomed to the new room layout.
Next Steps for Caregivers
If you're just starting, begin with the "low-hanging fruit": clear the 6-foot radius around the bed and move the mattress to the floor if possible. Once those are in place, move toward exit security with door alarms and window locks.
If you've implemented these changes and injuries are still occurring, it's time to look into clinical interventions. A sleep specialist can determine if pharmacological options, like low-dose clonazepam, are appropriate for high-risk cases. Remember to test your alarms weekly-a safety device is only useful if it actually works when the episode happens.
11 Comments
william wang
April 17 2026
Putting the mattress on the floor is a total game changer for peace of mind. I've seen this work wonders in clinical settings too, and it's way more practical than spending a fortune on rails that might just give someone something to climb over anyway.
Agatha Deo
April 17 2026
Oh, please. Only a complete amateur would think a "Sleep Guardian Pro" is the solution. It's obviously just another data-harvesting tool disguised as a medical device, probably sending your sleep patterns straight to a corporate server in the cloud while you're "safely" asleep. Truly naive.
Tama Weinman
April 19 2026
The suggestion about scheduled awakenings is cute, but let's be real, it only works for people who actually have their lives together enough to keep a sleep diary for two weeks. Most people are too disorganized for that, so they'll just keep ignoring the root cause while rearranging their furniture like it's a puzzle.
Richard Moore
April 19 2026
The floor mattress idea is spot on! 💯 Definitely saves a lot of stress. But man, if someone tries to push those secondary window locks, they're gonna need some serious grip strength! 🦾 Let's just keep the kids safe! 🇺🇸
Nell O'Leary
April 20 2026
The emphasis on sleep architecture is crucial here. By optimizing the circadian rhythm and minimizing cortisol spikes before bed, you're effectively reducing the probability of partial arousals. It's all about that homeostatic sleep drive (^_^)v
Cheryl C
April 21 2026
I tried the foam padding stuff and it totaly works lol!! Just make sure u get the thick stuff or it's useless 🤣 keep our kids safe in the laaaaand of the free!! 🇺🇸🎆
Rob Schlautman
April 23 2026
the whole idea of a six foot no fly zone is just so dramatic and honestly who has a room that big in this economy anyway because most of us are living in shoeboxes and trying to implement these high end safety measures just seems like a lot of work for something that might not even happen and the writing here is just so clinical it feels like a manual for a padded cell rather than a home
Adele Shaw
April 23 2026
My child used to walk every single night and it was a nightmare. I felt so alone in the struggle. The ground floor move was the only thing that actually stopped the panic attacks I had every time I heard a floorboard creak.
Dana Chichirita Nicoleta
April 24 2026
This guide is absolutely magnificent and provides such a wonderful sense of hope for families struggling with these terrifying nighttime episodes! I can only imagine the sheer relief a parent feels when they finally create a sanctuary where their precious little ones can sleep without danger, and the idea of letting children help build their "safety fort" is simply the most heartwarming approach to medical safety I have ever encountered in my entire life!
Nathan Berlin
April 25 2026
Imagine thinking you need a specialized alarm when basic common sense is free 🙄 we have better systems in India anyway 🇮🇳🔥 just use your brain instead of buying expensive gadgets from the west lol
Jon lee
April 26 2026
If anyone is feeling overwhelmed by the list of modifications, just remember to take it one step at a time. Starting with the floor mattress is a great way to get an immediate win without spending a lot of money. You've got this!