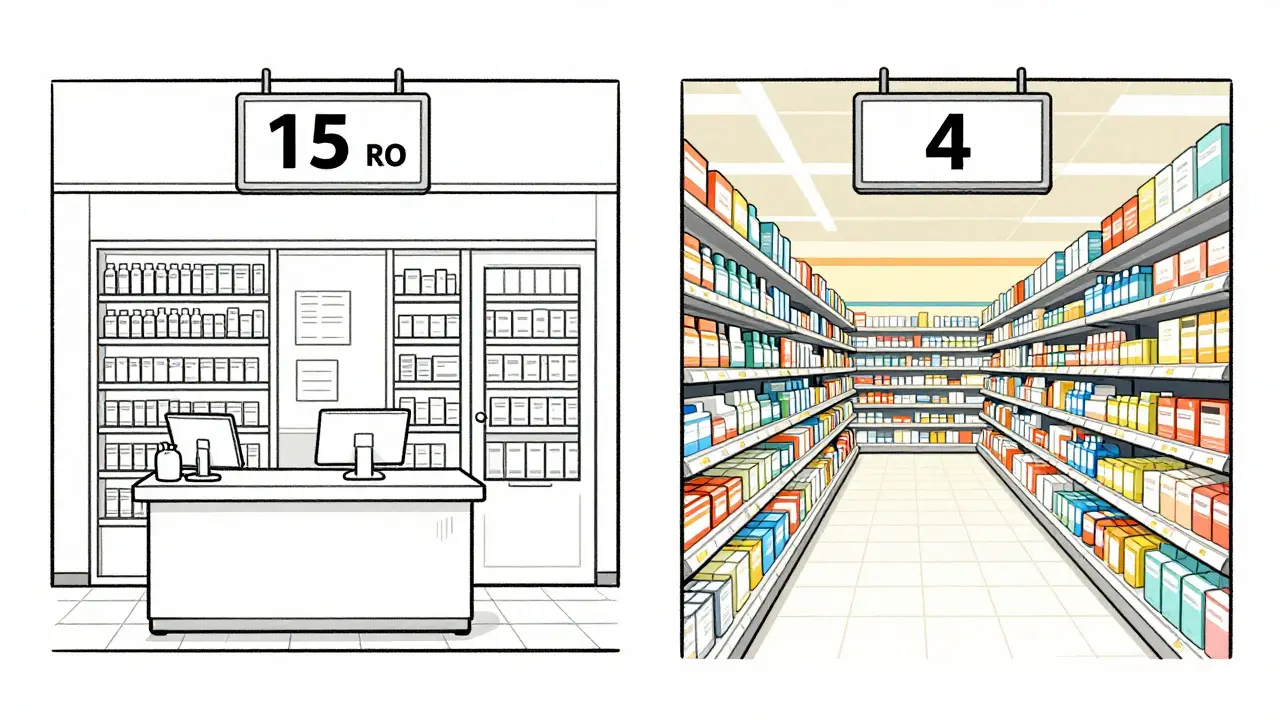
Imagine walking into a pharmacy in Germany and paying €15 for a month's supply of generic lisinopril, only to find out that the exact same medication costs just $4 at a Walmart in the US. It sounds backwards, right? We usually hear that the US has the most expensive healthcare in the world, but when it comes to generic drug prices is the cost of off-patent medications produced by multiple manufacturers, the US is often the cheapest place to be. While Americans pay a massive premium for new, brand-name drugs, they actually pay significantly less for the generics that make up the bulk of their prescriptions.
The Strange Paradox of Drug Pricing
It is a weird dichotomy. On one hand, the US is essentially the world's piggy bank for pharmaceutical innovation. Because the US government doesn't strictly cap the prices of new drugs, pharmaceutical companies make a huge portion of their profits here. On the other hand, once a drug's patent expires and it becomes a generic, the US market turns into a cutthroat battlefield where prices plummet.
According to data from the U.S. Department of Health and Human Services (ASPE), unbranded generics in the US are, on average, about 67% of the price found in 33 other OECD countries. That means Americans pay roughly one-third less for their generic meds than people in Europe. To put that in perspective, unbranded generics account for a staggering 90% of all prescriptions filled in the US. In Europe, that number is much lower-only about 41% of prescription volume is for unbranded generics. This lack of volume in Europe means there is less competitive pressure, which keeps the prices higher.
How the US Squeezes Generic Prices Down
Why is the US so much better at driving down generic costs? It comes down to the machinery of the healthcare system. In the US, we have Pharmacy Benefit Managers (or PBMs), which are third-party administrators who manage prescription drug benefits for health plans. These PBMs use their massive buying power to negotiate deep discounts and rebates from manufacturers.
When you combine PBMs with the sheer scale of giant pharmacy chains, you get a system of volume purchasing that forces generic manufacturers to compete on price. Sometimes, they compete so hard that prices actually drop below the cost of making the drug. This sounds great for the consumer, but it creates a hidden risk: when a drug becomes too cheap to be profitable, manufacturers simply stop making it, leading to the medicine shortages we occasionally see in US news cycles.
| Feature | United States | European Union (General) |
|---|---|---|
| Generic Market Volume | High (~90% of prescriptions) | Moderate (~41% of prescriptions) |
| Generic Pricing | Typically Lower (Competitive) | Typically Higher (Regulated) |
| Brand-Name Pricing | Very High (Market-driven) | Lower (Government negotiated) |
| Price Control Method | PBM negotiations & Market competition | Reference pricing & Health agencies (e.g., NICE) |
The European Approach: Stability Over Competition
Europe does things differently. Instead of letting a few giant companies negotiate prices, most European governments use Reference Pricing. This is a system where a government sets a maximum price for a drug based on what other similar countries are paying. If Germany sees that France is paying a certain amount for a generic, they'll peg their price to that.
In the UK, the National Institute for Health and Care Excellence (or NICE) looks at the cost-effectiveness of a drug before deciding if the government will pay for it. This keeps brand-name drugs affordable for the average citizen, but it also means there isn't the same "race to the bottom" that you see in the US generic market. Because the prices are more stable and predictable, manufacturers don't feel the need to slash prices to the same extent as they do in the US.
Who is Really Paying for Innovation?
This lead to a controversial point often debated by economists: the "free rider" problem. Because European countries negotiate brand-name drugs down to a fraction of the US price, the US effectively subsidizes global pharmaceutical R&D. Research suggests that about two-thirds of global drug discovery funding comes from the high revenues generated in the US market.
Essentially, US patients pay more for the "new stuff" (the brand-name drugs), which funds the research and development of the next generation of medicine. Once that patent expires, the US market aggressively drives the price down, making those drugs cheap for everyone. European systems benefit from the innovation funded by the US, but they don't have the same aggressive generic price-slashing mechanisms.
Real-World Impacts on the Patient
If you're a patient with a standard insurance plan in the US, your experience with generics is usually very smooth. In 49 states, pharmacists can automatically switch you to a generic version of a drug unless the doctor specifically forbids it. For many Medicare Part D users, a generic might only cost a few dollars, or even be free.
In Europe, the experience varies. In Germany, pharmacists have similar substitution powers. However, in France, a doctor often needs to give the green light for a switch to a generic. While European patients generally have lower out-of-pocket costs for expensive brand-name drugs, they often pay a fixed co-pay for generics that can actually be higher than the cost of the same generic in the US.
Is the Gap Closing?
We are seeing some shifts in the wind. The Inflation Reduction Act in the US is a game-changer. For the first time, Medicare is actually negotiating prices for some of the most expensive brand-name drugs. This is an attempt to bring US brand-name prices closer to the international average.
There have also been discussions about "Most Favored Nation" pricing, where the US would refuse to pay more for a drug than the lowest price paid by other developed nations. If this ever happened on a large scale, it would shake the entire global industry. Pharmaceutical companies would likely respond by raising prices in Europe to make up for the lost revenue in the US.
Why are generics cheaper in the US than in Europe?
The US has a much larger volume of generic prescriptions (about 90% of all fills) and a more aggressive competitive market. Pharmacy Benefit Managers (PBMs) and large pharmacy chains use their massive buying power to negotiate prices down to extremely low levels, often far lower than the government-set reference prices used in Europe.
Do US patients pay more for all drugs?
No. While Americans pay significantly more for brand-name (patented) medications-sometimes 3 to 4 times more than in OECD countries-they typically pay less for unbranded generic medications than people in Europe.
What is a PBM and how does it affect pricing?
A Pharmacy Benefit Manager (PBM) acts as a middleman between insurance companies, pharmacies, and drug manufacturers. They negotiate rebates and discounts. In the generic market, their ability to steer huge volumes of patients toward the cheapest possible generic helps drive those prices down for the consumer.
Does the US subsidize global drug research?
Many experts argue yes. Because the US allows higher prices for brand-name drugs, pharmaceutical companies make most of their R&D profits here. This funding supports the development of new medicines that are eventually used worldwide, including in countries with strict price controls.
Why do drug shortages happen if generics are so cheap?
When competition becomes too intense, the price of a generic can fall below the cost of manufacturing. At that point, companies stop producing the drug because it's no longer profitable. If only one or two companies are left and they also exit, a shortage occurs, which can ironically lead to a price spike by the last remaining supplier.
Next Steps for the Curious
If you're trying to manage your own medication costs, there are a few things you can do. In the US, always ask your pharmacist if a generic version is available and check if your insurance prefers one generic manufacturer over another to avoid higher co-pays. If you're in Europe, check your local regulations on pharmacist substitution, as some countries allow your pharmacist to save you money without needing a new prescription from your doctor.
8 Comments
David Snyder
April 14 2026
It's actually pretty heartening to see that generic competition is working so well for people. Even if the brand-name stuff is pricey, having those affordable options for the bulk of prescriptions is a huge win for accessibility.
S.A. Reid
April 15 2026
One must consider the possibility that these ostensibly 'cheap' generics are merely a facade for a more sinister coordination between PBMs and the state. It is quite probable that the perceived savings are simply a mechanism to maintain a dependent population while the true profits are sequestered in offshore accounts beyond the reach of any regulatory body. The notion that market competition naturally lowers prices is a charmingly naive interpretation of a system designed by the elite to consolidate power under the guise of consumer benefit.
Randy Ryder
April 16 2026
The vertical integration of PBMs into the healthcare stack creates some wild externalities. When you have this kind of monopsony power in the procurement phase, it fundamentally shifts the equilibrium for the manufacturers. I wonder if the current legislative shift toward Medicare negotiation will create a similar ripple effect in the generic pipeline or if that's strictly a brand-name phenomenon.
Billy Wood
April 17 2026
Keep fighting for lower prices!!! Love to see it!!!
rupa das
April 17 2026
basically just a way for the us to pretend they care about healthcare while still letting big pharma fleece the poor
Ikram Khan
April 19 2026
This is such an eye-opener!! 😲 I never realized the US was basically funding the world's medicine R&D like this! It's honestly wild how different the systems are! 🤯
Brooke Mowat
April 20 2026
Such a funky way to look at the world!!
It's like we're all just tiny pieces in this giant pharma puzzle, right? Just keep vibing with the cheap meds and hope the big brain research keeps flowing across the pond. Totally wild how we all just accept this weird dance of money and medz!!
Milo Tolley
April 20 2026
The supply chain volatility is an absolute nightmare!!! We're talking about total systemic failure when a drug becomes sub-profitable!!! The arbitrage between the US and EU markets is just a chaotic mess of rebate traps and formulary gymnastics!!! Absolutely tragic!!!